|
Surgeons should advise the parents about the possibility of loss of reduction and need for later surgical intervention. Circumferential casting and extreme manoeuvres of flexion should be avoided to prevent vascular and neurological compromises ( 9, 23). In case of no rotational deformity, coronal malalignment or significant extension of distal fragment (type IIA according to Wilkins ( 19)) this injury may potentially be treated nonoperatively ( 20- 22) with close reduction and casting. In a Gartland type II fracture the anterior humeral line is interrupted and the posterior cortex in hinged. Larger diameter pins should be adopted in order to obtain better stability and maintain reduction and alignment of the fracture. In case of varus at the fracture site more than 10°, compared to contralateral limb, close reduction and percutaneous pinning should be strongly considered ( 2). A type I fracture with medial compression should be reduced with external manoeuvres under general anaesthesia preventing the cubitus varus. 
A pitfall in the treatment of Gartland type I fracture lies in not recognizing medial impaction that could result in a varus deformity, which will not correct with growth ( 18). These injuries simply require immobilization for comfort and protection long-term outcome is usually excellent ( 16, 17). The treatment is not surgical, in a long arm cast with the elbow in 60-90° of flexion for approximately 3 weeks ( 15). Anterior humeral line is intact and the fracture displacement is less than 2 mm. These fractures are by definition stable fractures with minimal risk of further displacement or angulation. A positive fat pad sign is suggestive of fracture even in case of absence of radiological fracture lines. Other parameters to evaluate are the alignment of anterior humeral line that should intersect the middle 1/3 of the capitellum, anterior and posterior fat pad sign as indicators of elbow effusion ( 8, 9). In case of doubts, related to individual variation of Baumann’s angle, radiographs of the contralateral elbow should be used for comparison. The position of the ossification centers is checked, considering that they appear in a predictable order: capitellum at 1 year of age, radial head and medial epicondyle at 4-5 years of age, trochlea and olecranon at 8-9 years of age and lateral condyle appear at 10 years od age ( 6).Īssess the Baumann’s angle on AP view: the angle between the humeral shaft line and the parallel line to the lateral condylar phisis should be approximately 75° ( 7). 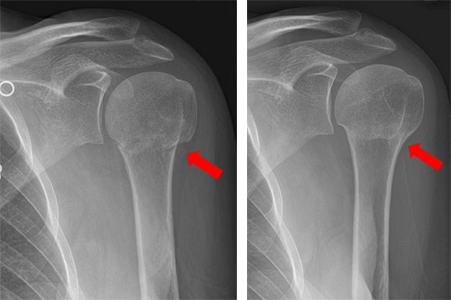
Often the pain limits flexion and extension manoeuvres of the articulation leading to difficulties in the interpretation of the images. 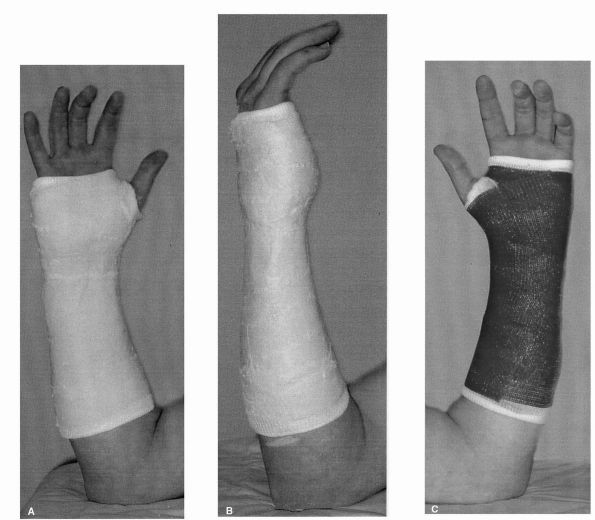
Antero-Posterior (AP) and a lateral view of the elbow should be performed in case of pain and tenderness after a trauma.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
